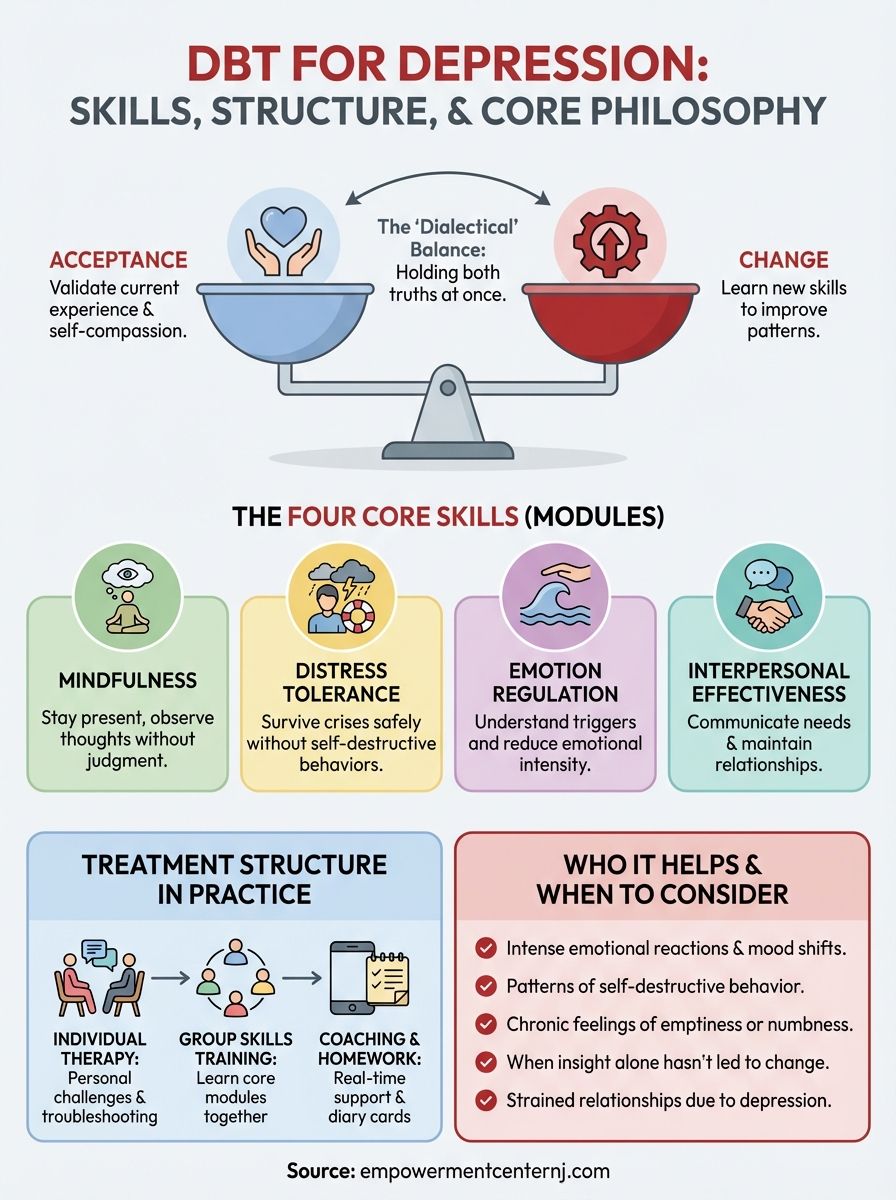
Dialectical Behavior Therapy is a structured treatment approach that teaches you how to manage intense emotions while accepting where you currently are. The word "dialectical" refers to the balance between two opposing ideas: accepting yourself as you are right now and working to change patterns that aren't serving you. This dual focus makes DBT particularly helpful when depression leaves you feeling stuck between self-criticism and hopelessness.
The core philosophy behind DBT
DBT operates on the principle that you can validate your current experience while still taking steps toward improvement. Unlike approaches that focus primarily on changing thoughts, DBT acknowledges that some situations genuinely are difficult and your feelings make sense given your circumstances. It teaches you to hold both truths at once, you deserve compassion for what you're going through, and you can develop skills to feel better.
You don't have to choose between accepting your depression and fighting to overcome it. DBT shows you how to do both simultaneously.
This philosophy matters because depression often comes with harsh self-judgment. When you criticize yourself for being depressed, you add another layer of suffering. DBT helps you practice self-compassion while building concrete skills, which breaks the cycle of feeling bad about feeling bad.
How CBT and DBT approach depression differently
Cognitive Behavioral Therapy focuses on identifying and changing the thought patterns that maintain your depression. You learn to notice negative automatic thoughts, challenge their accuracy, and replace them with more balanced perspectives. CBT treats thoughts as primary drivers of your emotional state, so changing how you think becomes the main goal.
DBT for depression takes a broader approach. Instead of focusing mainly on thought patterns, it teaches you four skill sets that address different aspects of emotional regulation. You learn mindfulness to stay present, distress tolerance to handle difficult moments, emotion regulation to understand and shift your feelings, and interpersonal effectiveness to improve relationships. These skills give you multiple entry points for managing depression rather than relying solely on cognitive restructuring.
The other major difference lies in acceptance versus change. CBT leans heavily toward change, teaching you to dispute distorted thinking and modify behaviors. DBT balances change strategies with validation and acceptance, recognizing that trying to change everything all at once can feel overwhelming when you're already depleted by depression.
The practical structure of DBT
Traditional DBT combines individual therapy with skills training in a group format. You meet with your therapist one-on-one to work through personal challenges and then attend weekly group sessions where you learn and practice the four core skill modules. Many programs also offer phone coaching between sessions so you can get support when you're actually experiencing a crisis.
Modified versions of DBT adapt this structure for different needs and settings. Some therapists integrate DBT skills into individual sessions without requiring group attendance. Others offer intensive outpatient programs that provide more frequent contact. The specific format matters less than learning the skills and having opportunities to practice them in real situations where your depression shows up.