You might assume that all therapy is basically the same, but the distinction between DBT and CBT directly affects what you'll learn, how you'll practice those skills, and whether you'll see the progress you're hoping for. Mismatched therapy can leave you feeling frustrated or stuck, not because therapy doesn't work, but because the approach doesn't align with what you're actually dealing with. Knowing which one fits your needs saves you time, energy, and the discouragement that comes from trying something that wasn't designed for your specific situation.
Different tools for different struggles
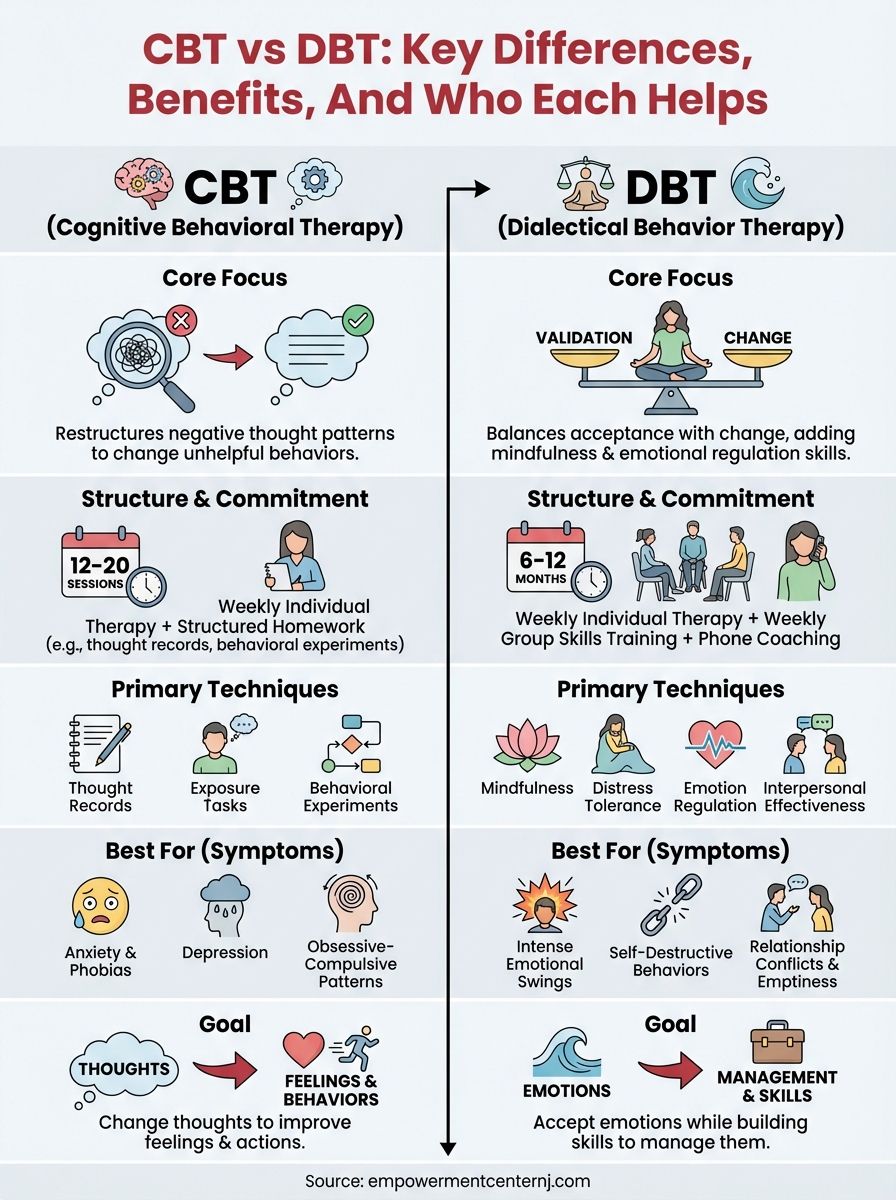
CBT gives you structured techniques to challenge negative thoughts and break cycles of anxiety or depression. If you find yourself catastrophizing, ruminating on past events, or avoiding situations because of feared outcomes, CBT offers direct solutions to rewire those patterns. You'll work through exercises that help you test your assumptions and build evidence against the distorted thinking that keeps you stuck.
DBT, on the other hand, was built for people who experience intense emotional swings that feel overwhelming and uncontrollable. If your emotions escalate quickly, if you struggle with self-destructive behaviors, or if relationships repeatedly end in conflict, DBT teaches emotional regulation and distress tolerance that CBT doesn't emphasize. It assumes that your emotions are valid but need better management, not just cognitive correction.
Choosing the wrong approach can delay your progress, while the right fit helps you build skills that actually address what's happening in your daily life.
Impact on your treatment experience
The structure of each therapy shapes how you spend your time in and outside of sessions. CBT typically runs shorter, maybe 12 to 20 sessions, with focused homework between meetings. You'll practice thought records, behavioral experiments, and exposure tasks that target specific symptoms. This works well if you have a clear problem to solve and prefer a direct, time-limited approach.
DBT requires a longer commitment and often includes group skills training alongside individual therapy. You'll learn mindfulness, interpersonal effectiveness, emotion regulation, and distress tolerance through weekly practice. The intensity and duration make sense when you're dealing with chronic emotional instability or patterns that have persisted for years. Understanding the dbt vs cbt difference helps you set realistic expectations about what you'll be asked to do and how long you'll need to commit.